Arch Iran Med. 27(4):216-222.
doi: 10.34172/aim.2024.31
Original Article
Clinicopathological Pattern of Endometrial Specimens in Women with Abnormal Uterine Bleeding and Ultrasonography Correlation
Mohadeseh Karimi Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing, 1, * 
Anahita Alizadeh Conceptualization, Formal analysis, Methodology, Supervision, Writing – review & editing, 1
Masoumeh Mahmoodi Data curation, 2
Author information:
1Department of Pathology, Faculty of Medicine, Hormozgan University of Medical Sciences, Bandar Abbas, Iran
2Department of Biostatistics, Hormozgan University of Medical Sciences, Bandar Abbas, Iran
Abstract
Background:
Abnormal uterine bleeding (AUB) refers to any symptomatic deviation from normal menstruation. AUB is a common gynecological disorder in non-pregnant women of reproductive age, accounting for approximately 33% of gynecological outpatient visits. The early diagnosis and management cause of AUB is important because of increased incidence of endometrial carcinoma with rapid growth. Transvaginal ultrasound is non-invasive imaging technique used to find endometrial carcinoma before referring patients for invasive techniques. Dilatation and curettage (D&C) and endometrial biopsy are surgical procedures that scrape the endometrial lining of the uterus for diagnosis and treatment. The aim of this study is to describe the clinicopathologic pattern of endometrial specimens in women with AUB and ultrasonographic correlation.
Methods:
Tissues from endometrial biopsy and curettage of 411 patients with AUB who referred to Shahid Mohammadi hospital were prospectively selected from 2021 to 2023. Patients were divided into three groups based on age and menstrual status including: premenopausal (18-39 years), perimenopausal (40-49 years) and postmenopausal (≥50 years). The results were correlated to patient’s age and other data and evaluated with statistical analysis.
Results:
During the two-year study period, a total of 411 endometrial specimens with clinical diagnosis of AUB were submitted and the results were analyzed. The youngest patient presenting with AUB was 21 years old, while the oldest was 77 years old. The most common complaint was menorrhagia in 201 (48.0%) out of 411 patients. The most common pathology finding in three groups was polyp in 100 (24.3%) cases. Hormonal effect was the next commonly observed pattern seen in 70 (17.0%) cases. P value was calculated as 0.003 which was significant using chi-square for the trend seen in age.
Conclusion:
Endometrial sampling is a useful tool for evaluation of women with AUB and referring patients for treatment. Histopathological evaluation of the endometrium is very useful in detecting the etiology of AUB. Transvaginal sonography has high sensitivity in detecting polyps.
Keywords: Abnormal uterine bleeding, Endometrium, Transvaginal sonography
Copyright and License Information
© 2024 The Author(s).
This is an open-access article distributed under the terms of the Creative Commons Attribution License (
https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article as: Karimi M, Alizadeh A, Mahmoodi M. Clinicopathological pattern of endometrial specimens in women with abnormal uterine bleeding and ultrasonography correlation. Arch Iran Med. 2024;27(4):216-222. doi: 10.34172/aim.2024.31
Introduction
In a normal menstrual cycle, with an interval of 28 ± 7 days and duration of 4 ± 3 days, blood loss is 30 to 80 mL/cycle. Abnormal uterine bleeding (AUB) refers to any symptomatic deviation of the following parameters from normal menstruation: frequency, regularity, duration, and volume. AUB includes various features and types such as oligomenorrhea, menorrhagia, menometrorrhagia, polymenorrhagia and spotting.1,2 In postmenopausal women, it is defined as any bleeding one year after menstruation stops.3 AUB is a common gynecological disorder in non-pregnant women of reproductive age, accounting for approximately 33% of gynecological outpatient visits.4 It may have a significant effect on women’s physical, social, emotional and material quality of life.5 In addition to the direct impact on women and their families, there is a huge cost to the economy and health services.6
The International Federation of Gynecology and Obstetrics (FIGO) classifies the etiology of AUB into 9 categories with a developed acronym PALM-COEIN. “PALM” refers to structural causes: Polyps; Adenomyosis; Leiomyomas; and Malignancy/Hyperplasia and “COEIN” refers to non-structural causes: Coagulopathy; Ovulatory dysfunction; Endometrial causes; Iatrogenic causes; Not Otherwise classified.7 In addition, long-term use of progestin-only contraceptives is associated with abnormal bleeding due to adverse effects on the endometrial microvasculature.8-10
Early diagnosis and management of the cause of AUB is important because the increased incidence of endometrial carcinoma with rapid growth is expected to reach 50% by 2040.11
Different diagnostic modalities can be used to diagnose the cause of AUB.12 Transvaginal ultrasound is a non-invasive imaging technique used to evaluate endometrial thickness, a marker and screening tool for endometrial carcinoma before referring patients for invasive techniques such as endometrial biopsy by dilatation and curettage (D&C).13 D&C and endometrial biopsy are important tools in diagnosis and treatment of AUB cases.14 D&C is a surgical procedure to scrape the endometrial lining of the uterus for diagnosis and treatment.15 Endometrial sampling is recommended for all women in perimenopausal age and above; especially, those at risk of atypical hyperplasia or carcinoma patients are selected for endometrial sampling to detect any histopathological atypia.16,17
The aim of this study is to describe the prevalence of different histopathological findings in endometrial specimens of AUB cases who underwent this procedure in our hospital over a 2-year period. We further compared histopathology findings with ultrasonography findings and clinical reports.
Materials and Methods
Using the formula Z21-alpha/2 pq/d2 = 3.84*0.25*0.75/0.0025 = 288 and taking into account the first type error of 5% and the precision of 5% and the information taken from the study by Bajithak et al, a sample size of 288 was calculated. In our study, tissues from endometrial biopsy and curettage of 411 patients with AUB who referred to Shahid Mohammadi hospital were prospectively selected from 2021 to 2023. An informed consent form was completed for each patient. The patient’s data including age, bleeding duration, menstruation period status and history of hormonal pill consumption, as well as para-clinical data including vaginal or pelvic ultrasonography and clinical reports were recorded. Patients were divided into three groups based on age and menstrual status including: premenopausal (18-39 years), perimenopausal (40-49 years) and postmenopausal (≥ 50 years). Endometrial specimens were processed and H&E slides were prepared and underwent microscopic examination by an expert pathologist. The results were correlated to the patient’s age and other data and evaluated with statistical analysis using SPSS (version 19) for Windows. The percentages of each pathologic condition in each age group and possible leading cause were reported. A P value less than 0.003 was considered significant. P values were calculated using F test.
Results
During the two-year study period, a total of 411 endometrial specimens with clinical diagnosis of AUB were submitted and the results were analyzed. The youngest patient presenting with AUB was 21 years old, while the oldest patient was 77 years old. Most patients were in the perimenopausal age group of 40-49 years, followed by the premenopausal age group of 21-39 years. Analysis of the distribution of births showed that most of women were multiparous (58.0%) and 7.0% of cases were nulliparous. The contraceptive methods used in the premenopausal and perimenopausal age groups were OCP in 90, condom in 100, IUD in 40, TL in 15, and natural in 73 cases.
The most common complaint was menorrhagia in 201 (48.0%) of 411 patients. The most common pathology finding in the study was polyp in 100 (24.3%) cases. Hormonal effect was the next most commonly observed pattern seen in 70 (17.0%) cases. Proliferative endometrium and inadequate sampling were reported in 53 (12.9%) and 48 (11.7%) cases, respectively. Secretory endometrium and disordered proliferative endometrium were found in 35 (8.5%) cases each. Endometrial hyperplasia was observed in 30 (7.3%) cases. Menstrual endometrium was found in 18 (4.4%) cases, and finally, menstrual anovulatory endometrium was seen in 11 (2.7%) cases (Table 1).
Table 1.
Demographic and Clinical Characteristics by Age Group (Main Variable)
|
Variables |
Perimenopausal No. (%)
|
Postmenopausal No. (%)
|
Premenopausal No. (%)
|
Total No. (%)
|
P
Value
|
| Secretory endometrium |
14 (3.4) |
6 (1.5) |
15 (3.6) |
35 (8.5) |
0.003 |
| Menstrual anovulatory endometrium |
7 (1.7) |
4 (1.0) |
0 (0.0) |
11 (2.7) |
| Endometrial hyperplasia |
12 (2.9) |
11 (2.7) |
7 (1.7) |
30 (7.3) |
| Polyp |
41 (10.0) |
20 (4.9) |
39 (9.5) |
100 (24.3) |
| Hormonal effect |
33 (8.0) |
8 (2.0) |
29 (7.0) |
70 (17.0) |
| Proliferative endometrium |
19 (4.6) |
6 (1.5) |
23 (5.6) |
48 (11.7) |
| Endometrial carcinoma |
0 (0.0) |
3 (0.7) |
0 (0.0) |
3 (0.7) |
| total |
126 (30.6) |
58 (14.3) |
113 (27.4) |
297 (72.2) |
Chronic endometritis was found in 5 (1.2%) cases. Endometrial carcinoma was seen in 3 (0.7%) cases. Atrophic endometrium was found in 2 (0.5%) cases and submucosal leiomyoma was seen in 1 (0.2%) case (Table 2).
Table 2.
Demographic and Clinical Characteristics by Age Group (Sub Variable).
|
Variables
|
Perimenopausal No. (%)
|
Postmenopausal No. (%)
|
Premenopausal No. (%)
|
Total No. (%)
|
P
Value
|
| Inadequate sample |
21 (5.1) |
21 (5.1) |
11 (2.7) |
53 (12.9) |
0.003 |
| Disordered proliferative endometrium |
13 (3.2) |
8 (1.9) |
14 (3.4) |
35 (8.5) |
| Shedding endometrium |
8 (1.9) |
4 (1.0) |
6 (1.5) |
18 (4.4) |
| Atrophic endometrium |
1 (0.2) |
1 (0.2) |
0 (0.0) |
2 (0.5) |
| Submucosal leiomyoma |
1 (0.2) |
0 (0.0) |
0 (0.0) |
1 (0.2) |
| Chronic endometritis |
1 (0.2) |
1 (0.2) |
3 (0.7) |
5 (1.2) |
| Total |
45 (10.8) |
35 (8.4) |
34 (5.6) |
114 (27.8) |
Polyp and proliferative endometrium were the most common patterns seen in the premenopausal group. In the perimenopausal group, polyp was the most common followed by hormonal effect. In the postmenopausal group, inadequate sampling was the most common pattern followed by polyp. Most of the endometrial and other carcinomas were found in the postmenopausal group (Table 1).
The most common abnormality reported by transvaginal sonography was thickened endometrium (46%), followed by endometrial polyp (27%), submucous myoma (10%), adenomyosis (2%), and malignancy (1%) (Table 3).
Table 3.
Causes of AUB Identified by Transvaginal Sonography
|
Findings
|
Number of Cases
|
Percent
|
| Thickened endometrium |
190 |
46 |
| Endometrial polyp |
112 |
27 |
| Submucosal leiomyoma |
41 |
10 |
| adenomyosis |
8 |
2 |
| malignancy |
4 |
1 |
| Ovary cyst |
12 |
3 |
| No abnormal findings |
45 |
11 |
Table 4 shows the overall sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) for transvaginal sonography in the diagnosis of uterine abnormalities. Transvaginal ultrasound had high sensitivity in detecting polyps. However, in leiomyoma, transvaginal ultrasound findings do not match histologically because the sample of endometrial biopsy and curettage is almost from the mucosal surface and not from the muscle layer.
Table 4.
Diagnostic Accuracy of TVS in AUB
|
Findings
|
Sensitivity (95% CI)
|
Specificity (95% CI)
|
PPV (95% CI)
|
NPV (95%CI)
|
| Thickened Endometrium |
82% (75.61% to 88.52%) |
23% (8.22% to 47.17%) |
64% (59.38% to 65.32%) |
25% (10.92% to 37.75%) |
| Polyp |
89% (83.68% to 92.51%) |
47% (28.34% to 65.67%) |
77% (73.63% to 79.47%) |
28% (22.76% to 37.32%) |
| Submucosal leiomyoma |
5% (0.63% to 17.32%) |
70% (57.10% to 82.37%) |
8% (2.96% to 33.90%) |
53% (46.71% to 55.90%) |
| Malignancy |
72% (61.78% to 81.15%) |
57% (40.82% to 73.69%) |
55% (47.63% to 61.32%) |
67% (56.63% to 78.32%) |
Microscopic examination of endometrial polyp, endometrial hyperplasia, endometrioid carcinoma, proliferative phase, secretory phase, menstrual phase and atrophic phase of endometrium showed various histological findings (Figures 1-9).
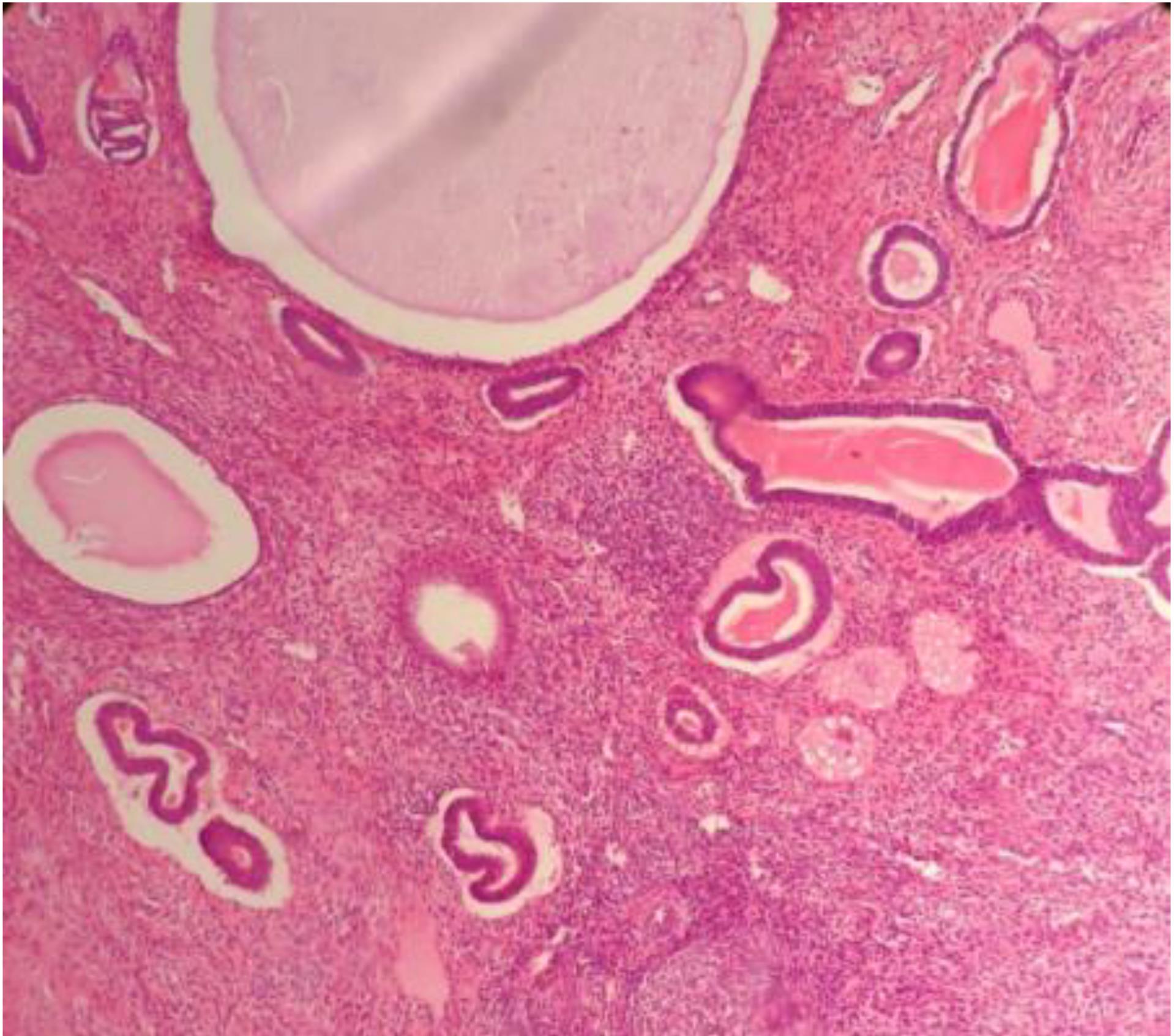
Figure 1.
Polyp: the photomicrograph shows cystically dilated glands along with compact stroma and thick wall blood vessels. Hematoxylin and eosin (H&E) stain (× 400)
.
Polyp: the photomicrograph shows cystically dilated glands along with compact stroma and thick wall blood vessels. Hematoxylin and eosin (H&E) stain (× 400)
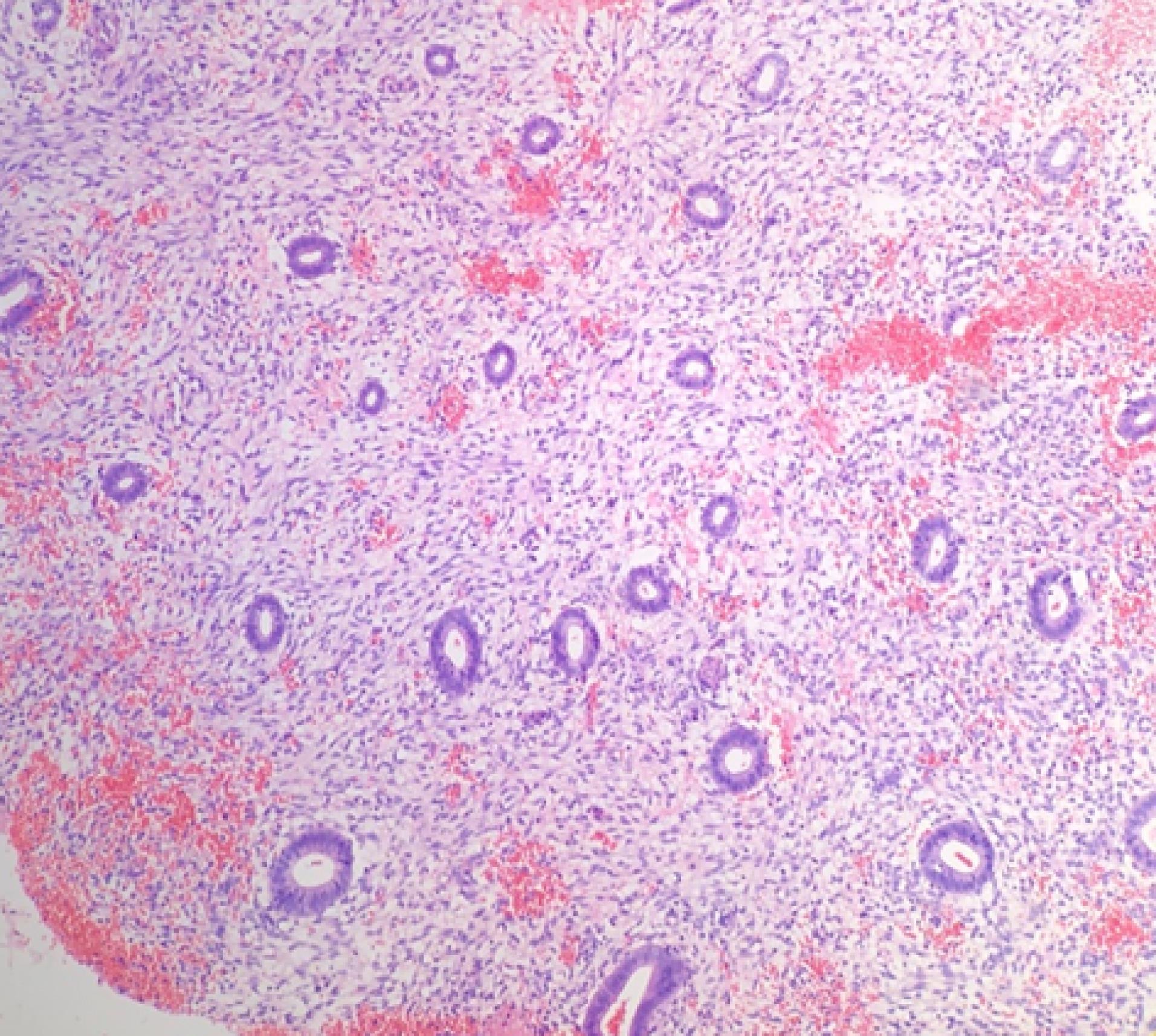
Figure 2.
Hormonal Effect: The photomicrograph shows small glands with abundant decidua. Hematoxylin and eosin (H&E) stain (× 400)
.
Hormonal Effect: The photomicrograph shows small glands with abundant decidua. Hematoxylin and eosin (H&E) stain (× 400)
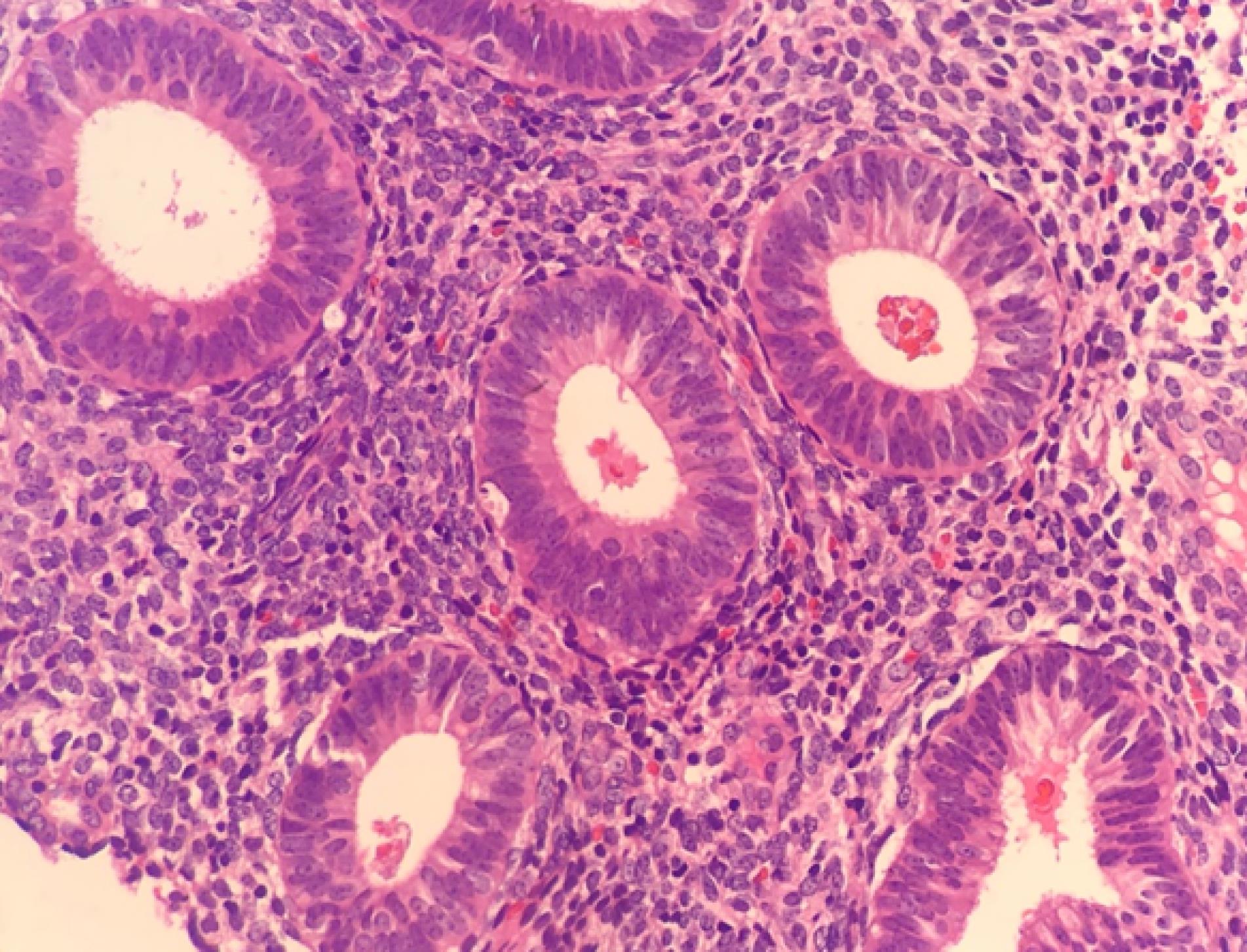
Figure 3.
Proliferative Endometrium: The photomicrograph shows uniform small glands along with compact stroma. Hematoxylin and eosin (H&E) stain (× 400)
.
Proliferative Endometrium: The photomicrograph shows uniform small glands along with compact stroma. Hematoxylin and eosin (H&E) stain (× 400)
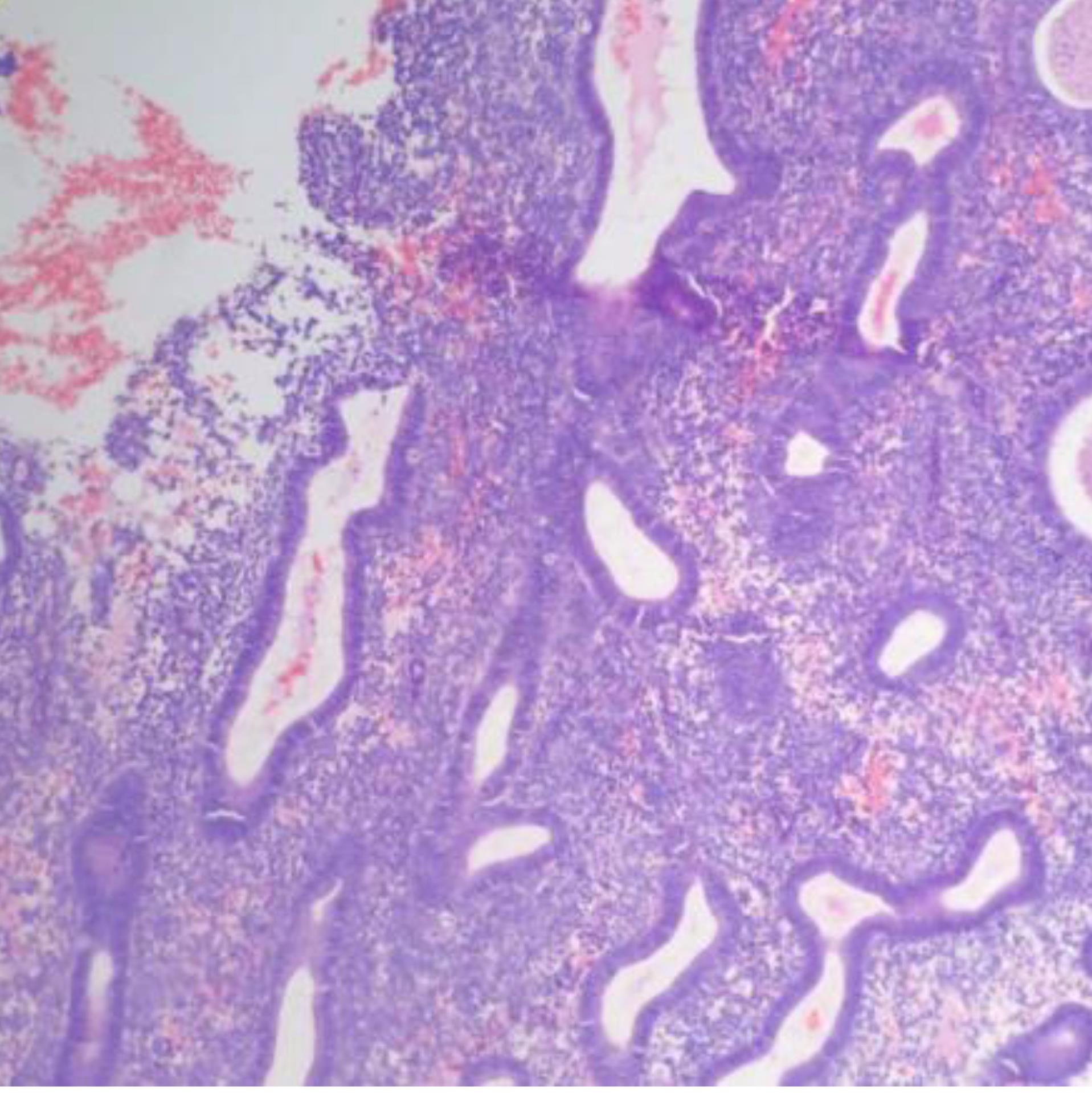
Figure 4.
Disordered Proliferative Endometrium: The photomicrograph shows disordered glandular proliferation with variably sized and shaped glands. Hematoxylin and eosin (H&E) stain (× 400).
.
Disordered Proliferative Endometrium: The photomicrograph shows disordered glandular proliferation with variably sized and shaped glands. Hematoxylin and eosin (H&E) stain (× 400).
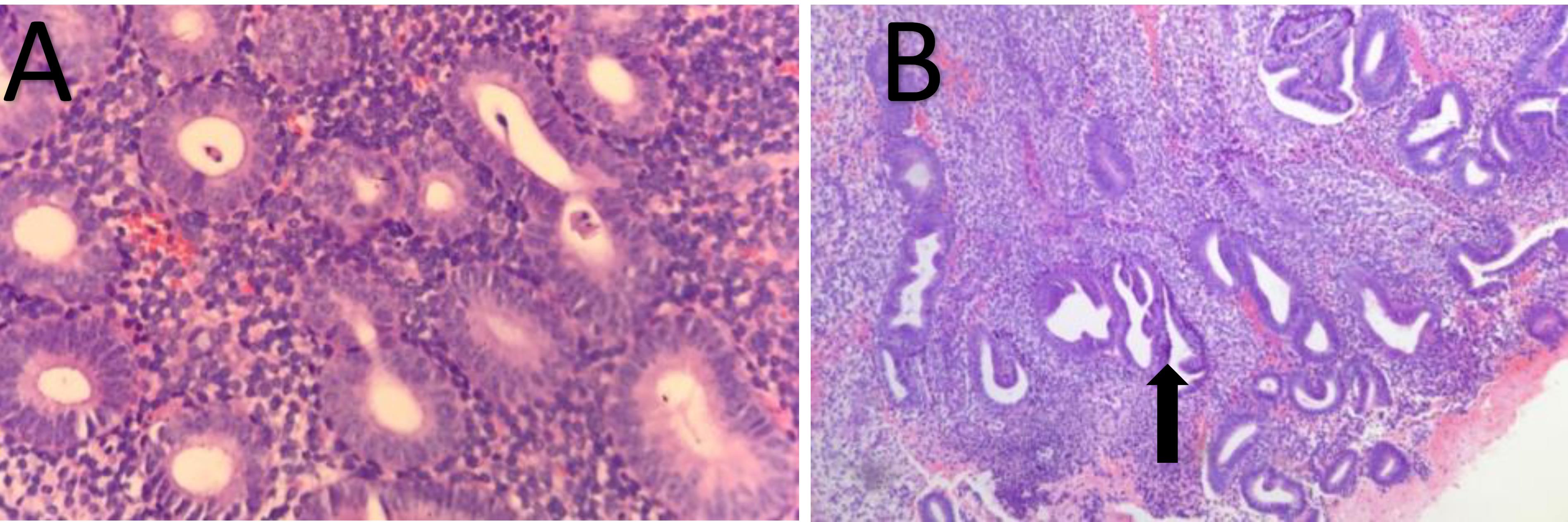
Figure 5.
Endometrial Hyperplasia: A) Glandular Proliferation in Compact Stroma; B) Crowded Glands with Branching. Hematoxylin and eosin (H&E) stain (× 400) (see black arrows)
.
Endometrial Hyperplasia: A) Glandular Proliferation in Compact Stroma; B) Crowded Glands with Branching. Hematoxylin and eosin (H&E) stain (× 400) (see black arrows)
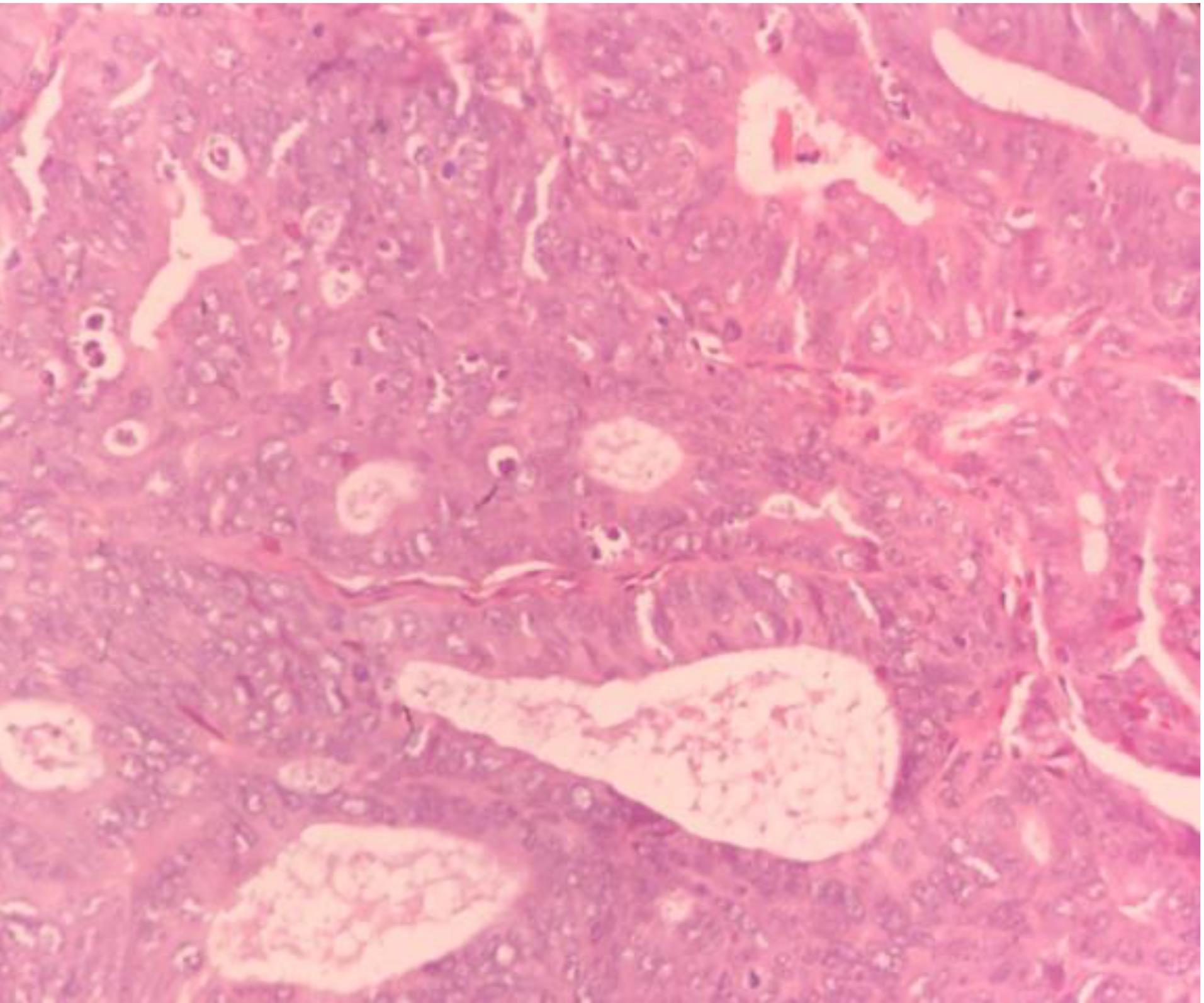
Figure 6.
Endometroid Carcinoma: The photomicrograph shows the neoplastic glands with back to back arrangement and nuclear pleomorphism, hyperchromatism and prominent nucleoli of epithelial lining. Hematoxylin and eosin (H&E) stain (× 400)
.
Endometroid Carcinoma: The photomicrograph shows the neoplastic glands with back to back arrangement and nuclear pleomorphism, hyperchromatism and prominent nucleoli of epithelial lining. Hematoxylin and eosin (H&E) stain (× 400)
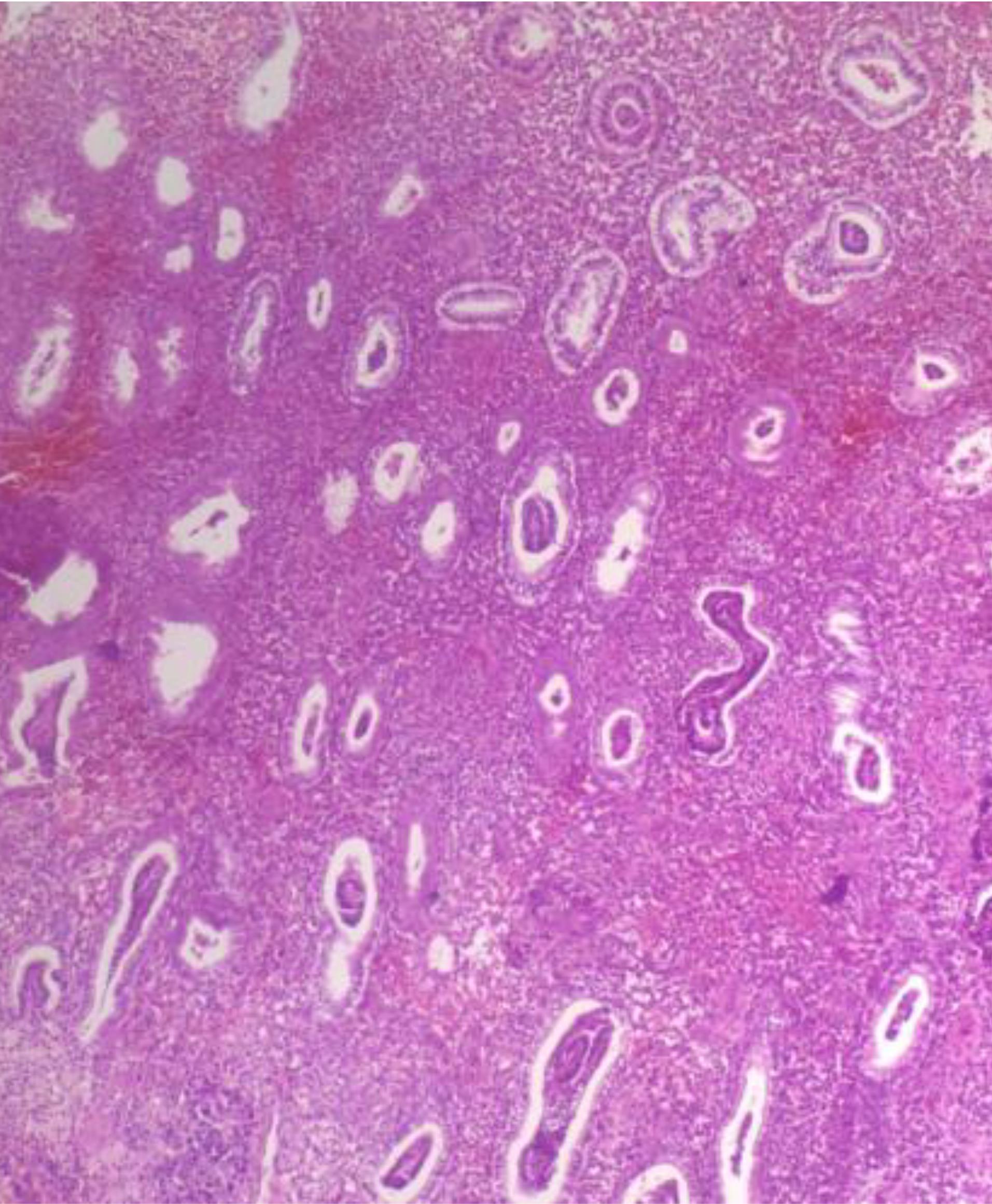
Figure 7.
Secretory Endometrium: The photomicrograph shows subnuclear vacuolation of glands along with mild stromal edema. Hematoxylin and eosin (H&E) stain (× 400)
.
Secretory Endometrium: The photomicrograph shows subnuclear vacuolation of glands along with mild stromal edema. Hematoxylin and eosin (H&E) stain (× 400)
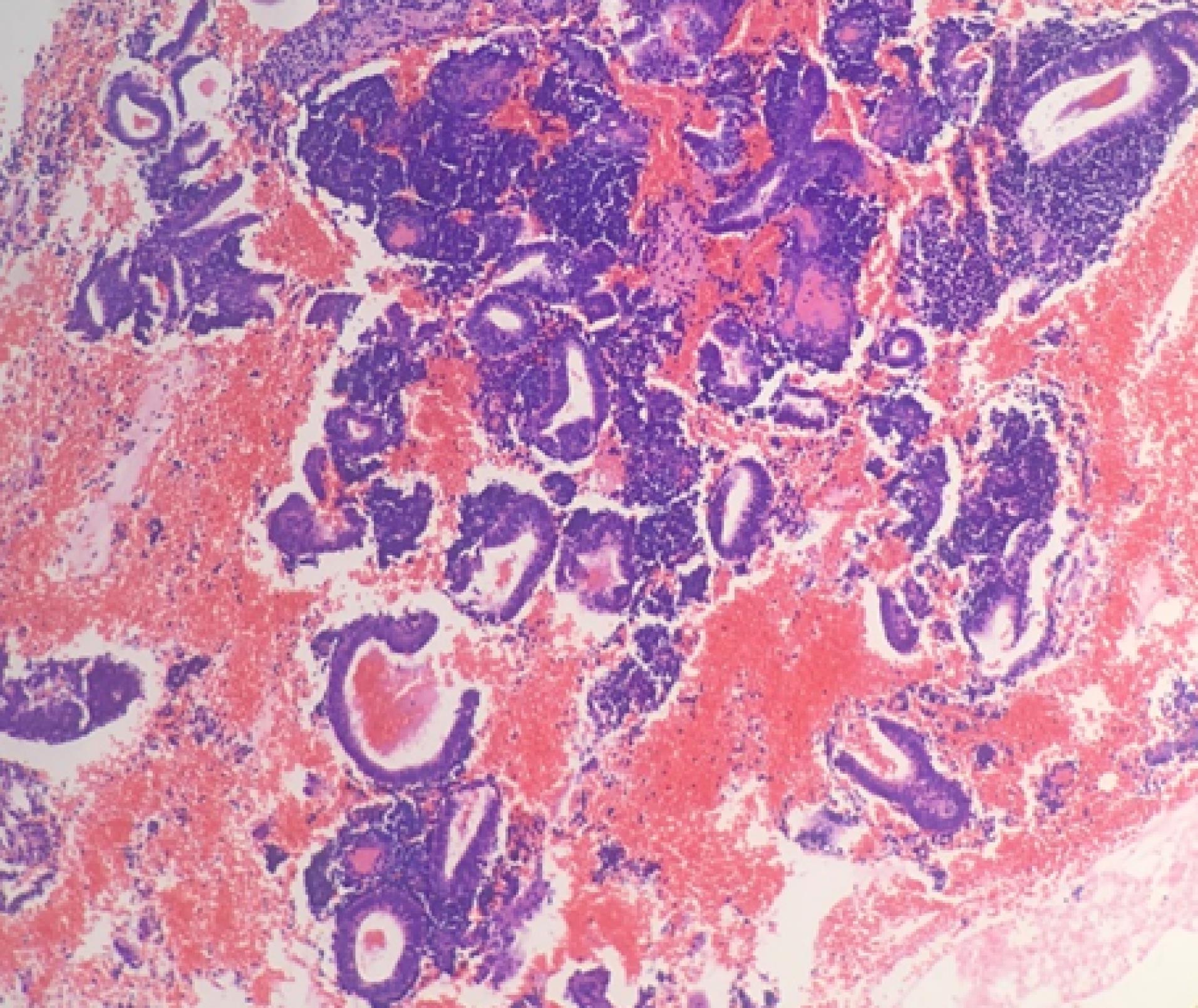
Figure 8.
Menstrual Endometrium: The photomicrograph shows broken and fragmented endometrial glands. Hematoxylin and eosin (H&E) stain (× 400)
.
Menstrual Endometrium: The photomicrograph shows broken and fragmented endometrial glands. Hematoxylin and eosin (H&E) stain (× 400)
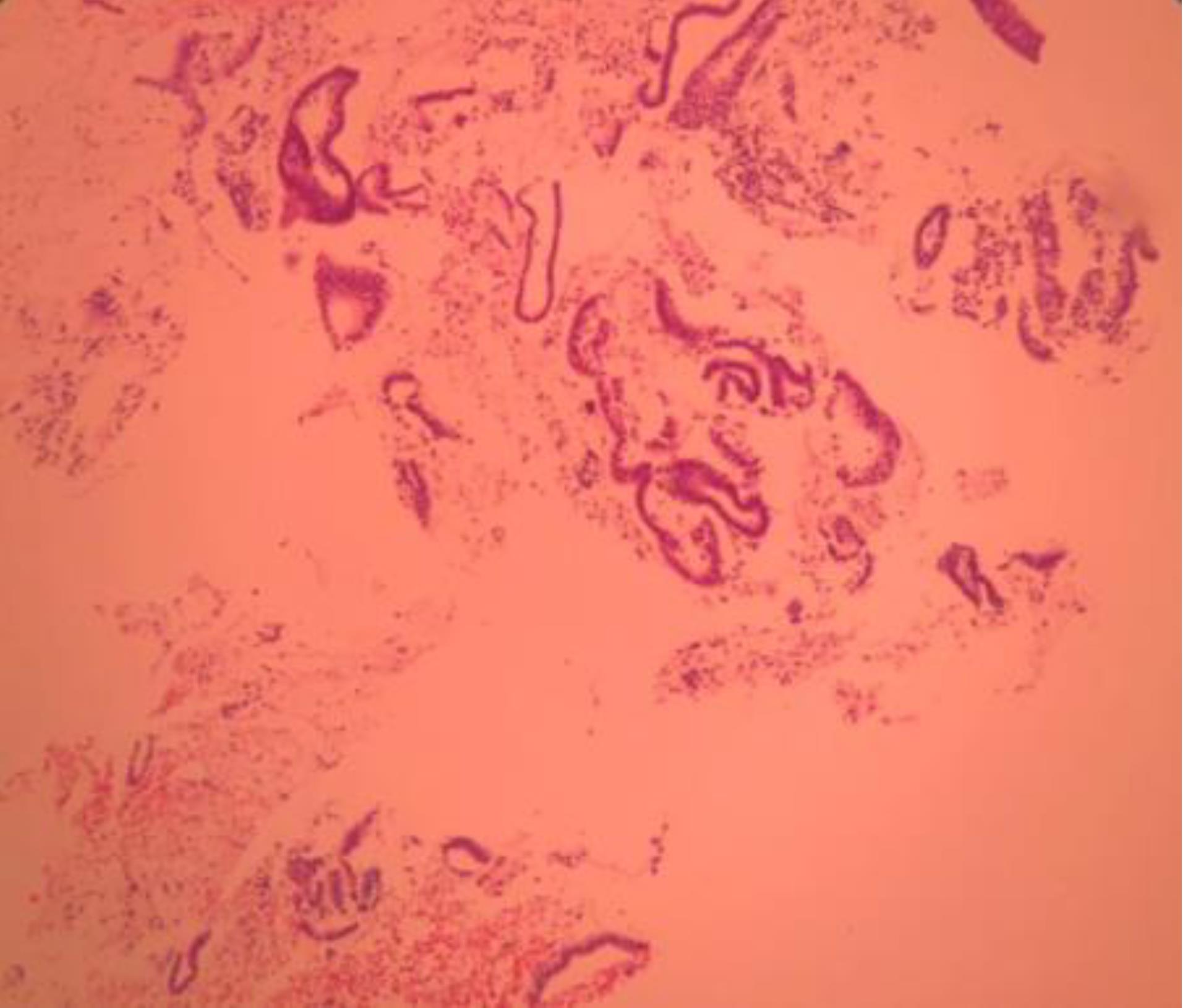
Figure 9.
Atrophic Endometrium: The photomicrograph shows multiples strips of mitotically inactive endometrial glands with flattened epithelium. Hematoxylin and eosin (H&E) stain (× 400)
.
Atrophic Endometrium: The photomicrograph shows multiples strips of mitotically inactive endometrial glands with flattened epithelium. Hematoxylin and eosin (H&E) stain (× 400)
Discussion
In this study, perimenopausal women constituted the most common age group for AUB (171 patients), followed by premenopausal women (147 patients). Other studies have found that AUB is most commonly found in perimenopausal women.18-24 Our study, and others, found the most common complaint of patient to be menorrhagia.18-22
In this study, preoperative transvaginal sonography was done to identify the cause of AUB. Transvaginal sonography is a practical and initial way to detect possible reasons for AUB. The findings of transvaginal sonography are shown in Table 3. The most common pathology finding in our study was polyps in 100 (24.3%) cases. Preoperative transvaginal sonography has high sensitivity for polyp detection.
The prevalence of polyps was reported in studies done by Lairah et al (40%).25 In a study by Dhruvi et al, endometrial polyps were found in 2% of women.1 A polyp is a focal hyperplastic overgrowth of endometrial glands and stroma around a vascular core in the uterine cavity.26 Possible etiologies include genetic, biochemical, and hormonal factors.27,28 In our study, it was related to OCP use in 17 (4.0%) patients.
Hormonal effect was the second most common histopathological finding identified in 75 women (18.2%) that was comparable with the study done by Alshdaifat et al (16.9%).3
We found endometrial hyperplasia in 30 (7.3%) women, most commonly in the perimenopausal age group (2.9%). In other studies, endometrial hyperplasia was found most commonly in the postmenopausal age group.29-35 Prolonged endogenous (chronic anovulation) or exogenous (hormone replacement therapy) estrogen can stimulate the glandular and stromal overgrowth that causes endometrial hyperplasia. Early diagnosis of endometrial hyperplasia is important as it may precede or coexist with endometrial cancer.36 Therefore, in the perimenopausal age group with AUB, any dangerous pathology findings should always be ruled out.
In our study, endometrial carcinoma was found in 3 (0.7%) women. This was comparable with the findings reported by Shah et al (0.3%),37 Gulia et al (1%),29 Vaidyea et al (1%),30 Mishra et al (2%)38 and Khan et al (2%).33
In this study, the mean age of patients who presented with postmenopausal bleeding was 62 years. The histological type of malignancy was endometrioid adenocarcinoma.
Previous studies have reported different incidence rates of endometrial carcinoma due to the variation in the geographical location, lifestyle, socioeconomic conditions, as well as their inclusion criteria.1
We found chronic endometritis in 5 (1.2%) women, most commonly seen in the premenopausal age group (0.7%), due to abortions, intra-uterine contraceptive devices, and ascending route of infections.
In the present study, 53 (12.9%) samples were insufficient for histopathological diagnosis. In a study by Alshdaifat et al, inadequate sampling was reported in 101 (51.8%) women.3
Endometrial sampling techniques used in our study were Pipelle and D&C. Pipelle causes less pain, less tissue volume and is more cost effective compared with D&C.39 In our study, inadequate sampling was most commonly seen with Pipelle (65%).
Endometrial sampling is a useful tool for evaluation of women with AUB and referring patients for treatment. Histopathological evaluation of the endometrium is very useful in detecting the etiology of AUB. Our histopathological analysis showed that the most common pattern in endometrial specimens of AUB cases was polyps, followed by hormonal effect and proliferative endometrium. Transvaginal sonography has high sensitivity in detecting polyps.
Acknowledgements
We wish to thank our counselors in the Clinical Research Center of Shahid Mohammadi hospital in Bandar Abbas.
Competing Interests
The authors declare no conflict of interest.
Data Availability Statement
The data sets used during the current study are available from the corresponding author on reasonable request.
Ethical Approval
Hormozgan University of Medical Sciences Ethical Committee approved the study under the ethical code IR.HUMS.REC.1401.208 and the study conforms with the Helsinki Declaration’s statements. Written informed consent was obtained from the patients for publication of this study and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Funding
The study did not receive any funding.
References
- Shah D, Savsaviya MJ, Patel NP. Histopathological spectrum of endometrium in hysterectomy specimens from cases of abnormal uterine bleeding. Int J Clin Diagn Pathol 2022; 5(1):11-6. doi: 10.33545/pathol.2022.v5.i1a.446 [Crossref] [ Google Scholar]
- Sohu DM, Das B, Rasul MR, Memon IK. Role of transvaginal ultrasound in management of abnormal uterine bleeding. Pak J Med Health Sci 2022; 16(5):127-8. doi: 10.53350/pjmhs22165127 [Crossref] [ Google Scholar]
- Alshdaifat EH, El-Deen Al-Horani SS, Al-Sous MM, Al-Horani S, Sahawneh FE, Sindiani AM. Histopathological pattern of endometrial biopsies in patients with abnormal uterine bleeding in a tertiary referral hospital in Jordan. Ann Saudi Med 2022; 42(3):204-13. doi: 10.5144/0256-4947.2022.204 [Crossref] [ Google Scholar]
- Iweha C, Graham A, Cui W, Marsh C, Nothnick WB. The uterine natural killer cell, cytotoxic T lymphocyte, and granulysin levels are elevated in the endometrium of women with nonstructural abnormal uterine bleeding. F S Sci 2022; 3(3):246-54. doi: 10.1016/j.xfss.2022.04.003 [Crossref] [ Google Scholar]
- National Institute for Health and Care Excellence (NICE). Clinical Guideline 44; Heavy Menstrual Bleeding. NICE; 2007. Available from: http://www.nice.org.uk/nicemedia/pdf/CG44FullGuidelin.pdf.
- Frick KD, Clark MA, Steinwachs DM, Langenberg P, Stovall D, Munro MG. Financial and quality-of-life burden of dysfunctional uterine bleeding among women agreeing to obtain surgical treatment. Womens Health Issues 2009; 19(1):70-8. doi: 10.1016/j.whi.2008.07.002 [Crossref] [ Google Scholar]
- Munro MG, Critchley HO, Broder MS, Fraser IS. FIGO classification system (PALM-COEIN) for causes of abnormal uterine bleeding in nongravid women of reproductive age. Int J Gynaecol Obstet 2011; 113(1):3-13. doi: 10.1016/j.ijgo.2010.11.011 [Crossref] [ Google Scholar]
- Rogers PA, Au CL, Affandi B. Endometrial microvascular density during the normal menstrual cycle and following exposure to long-term levonorgestrel. Hum Reprod 1993; 8(9):1396-404. doi: 10.1093/oxfordjournals.humrep.a138268 [Crossref] [ Google Scholar]
- Hickey M, Fraser I, Dwarte D, Graham S. Endometrial vasculature in Norplant users: preliminary results from a hysteroscopic study. Hum Reprod 1996; 11 Suppl 2:35-44. doi: 10.1093/humrep/11.suppl_2.35 [Crossref] [ Google Scholar]
- Runic R, Schatz F, Wan L, Demopoulos R, Krikun G, Lockwood CJ. Effects of Norplant on endometrial tissue factor expression and blood vessel structure. J Clin Endocrinol Metab 2000; 85(10):3853-9. doi: 10.1210/jcem.85.10.6856 [Crossref] [ Google Scholar]
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2018; 68(6):394-424. doi: 10.3322/caac.21492 [Crossref] [ Google Scholar]
- Veena BT, Shivalingaiah N. Role of transvaginal sonography and diagnostic hysteroscopy in abnormal uterine bleeding. J Clin Diagn Res 2014; 8(12):Oc06-8. doi: 10.7860/jcdr/2014/8813.5236 [Crossref] [ Google Scholar]
- Maiti G, Lele P, Borse D. Comparison of transvaginal sonography with hysteroscopy and correlation with histopathological report in case of abnormal uterine bleeding. Int J Reprod Contracept Obstet Gynecol 2018; 7(2):710-4. doi: 10.18203/2320-1770.ijrcog20180199 [Crossref] [ Google Scholar]
- Singh A, Arora AK. Why hysterectomy rate are lower in India. Indian J Community Med 2008; 33(3):196-7. doi: 10.4103/0970-0218.42065 [Crossref] [ Google Scholar]
- Trinder J, Brocklehurst P, Porter R, Read M, Vyas S, Smith L. Management of miscarriage: expectant, medical, or surgical? Results of randomised controlled trial (miscarriage treatment (MIST) trial). BMJ 2006; 332(7552):1235-40. doi: 10.1136/bmj.38828.593125.55 [Crossref] [ Google Scholar]
- Singh S, Best C, Dunn S, Leyland N, Wolfman WL. No 292-Abnormal uterine bleeding in pre-menopausal women. J Obstet Gynaecol Can 2018; 40(5):e391-415. doi: 10.1016/j.jogc.2018.03.007 [Crossref] [ Google Scholar]
- Farquhar CM, Lethaby A, Sowter M, Verry J, Baranyai J. An evaluation of risk factors for endometrial hyperplasia in premenopausal women with abnormal menstrual bleeding. Am J Obstet Gynecol 1999; 181(3):525-9. doi: 10.1016/s0002-9378(99)70487-4 [Crossref] [ Google Scholar]
- Jyotsana MK, Sharma S. Role of hysteroscopy and laparoscopy in evaluation of abnormal uterine bleeding. JK Sci 2004; 6(1):23-7. [ Google Scholar]
- Muzaffar M, Akhtar KA, Yasmin S, Mahmood Ur R, Iqbal W, Khan MA. Menstrual irregularities with excessive blood loss: a clinico-pathological correlation. J Pak Med Assoc 2005; 55(11):486-9. [ Google Scholar]
- Doraiswami S, Johnson T, Rao S, Rajkumar A, Vijayaraghavan J, Panicker VK. Study of endometrial pathology in abnormal uterine bleeding. J Obstet Gynaecol India 2011; 61(4):426-30. doi: 10.1007/s13224-011-0047-2 [Crossref] [ Google Scholar]
- Bhosle A, Fonseca M. Evaluation and histopathological correlation of abnormal uterine bleeding in perimenopausal women. Bombay Hosp J 2010; 52(1):69-72. [ Google Scholar]
- Khan S, Hameed S, Umber A. Histopathological pattern of endometrium on diagnostic D & C in patients with abnormal uterine bleeding. Ann King Edw Med Univ 2011; 17(2):166-70. doi: 10.21649/akemu.v17i2.293 [Crossref] [ Google Scholar]
- Sinha P, Rekha PR, Konapur PG, Thamilsevi R, Subramaniam PM. Pearls and pitfalls of endometrial curettage with that of hysterectomy in DUB. J Clin Diagn Res 2011; 5(6):1199-202. [ Google Scholar]
- Azim P, Khan MM, Sharif N, Khattak EG. Evaluation of abnormal uterine bleeding on endometrial biopsies. Isra Med J 2011; 3(3):84-8. [ Google Scholar]
- UNTAO. Correlation Between Transvaginal Sonography, Hysteroscopic and Histopathological Findings in Patients with Abnormal Uterine Bleeding at Southern Philippines Medical Center. Available from: https://seud.org/wp-content/uploads/2022/2022_SEUD_POSTERS/UNTAO.pdf.
- Savelli L, De Iaco P, Santini D, Rosati F, Ghi T, Pignotti E. Histopathologic features and risk factors for benignity, hyperplasia, and cancer in endometrial polyps. Am J Obstet Gynecol 2003; 188(4):927-31. doi: 10.1067/mob.2003.247 [Crossref] [ Google Scholar]
- Vanni R, Dal Cin P, Marras S, Moerman P, Andria M, Valdes E. Endometrial polyp: another benign tumor characterized by 12q13-q15 changes. Cancer Genet Cytogenet 1993; 68(1):32-3. doi: 10.1016/0165-4608(93)90070-3 [Crossref] [ Google Scholar]
- Liu Z, Kuokkanen S, Pal L. Steroid hormone receptor profile of premenopausal endometrial polyps. Reprod Sci 2010; 17(4):377-83. doi: 10.1177/1933719109356803 [Crossref] [ Google Scholar]
- Gulia SP, Lavanya M, Chaudhury M, Kumar SP. Study of endometrial pathology in cases of abnormal uterine bleeding – a meta-analysis of 435 cases. J Med Sci Technol 2013; 2(3):124-29. [ Google Scholar]
- Vaidya S, Vaidya SA. Patterns of lesions in hysterectomy specimens in a tertiary care hospital. JNMA J Nepal Med Assoc 2015; 53(197):18-23. [ Google Scholar]
- Shah FR, Thaker GS, Shah JM. Clinico-histopathological analysis in patients with abnormal uterine bleeding. Natl J Integr Res Med 2016; 7(5):14-7. [ Google Scholar]
- Singh N, Sonawane S. Spectrum of endometrial pathology in abnormal uterine bleeding. Int J Health Sci Res 2017; 7(9):28-34. [ Google Scholar]
- Doraiswami S, Johnson T, Rao S, Rajkumar A, Vijayaraghavan J, Panicker VK. Study of endometrial pathology in abnormal uterine bleeding. J Obstet Gynaecol India 2011; 61(4):426-30. doi: 10.1007/s13224-011-0047-2 [Crossref] [ Google Scholar]
- Bharati M, Bhol SK. Study of clinical and pathological correlation of AUB patients undergoing hysterectomy. Int J Gynaecol 2017; 3:13-8. [ Google Scholar]
- Pradhan SB, Sedhain M, Acharya S, Maharjan S, Regmi S. Clinico-pathological study of hysterectomy specimens in Kathmandu Medical College Teaching Hospital. Birat J Health Sci 2018; 3(2):423-6. doi: 10.3126/bjhs.v3i2.20938 [Crossref] [ Google Scholar]
- Corniţescu FI, Tănase F, Simionescu C, Iliescu D. Clinical, histopathological and therapeutic considerations in non-neoplastic abnormal uterine bleeding in menopause transition. Rom J Morphol Embryol 2011; 52(3):759-65. [ Google Scholar]
- Shah R, Dayal A, Kothari S, Patel S, Dalal B. Histopathological interpretation of endometrium in abnormal uterine bleeding Int J Med Sci Public Health. 2014,452-56 2014; 3(4):452-6. doi: 10.5455/ijmsph.2014.120220142 [Crossref] [ Google Scholar]
- Sudhamani S, Sunila Sunila, Sirmukaddam S, Agrawal D. Clinicopathological study of abnormal uterine bleeding in perimenopausal women. J Sci Soc 2015; 42(1):3-6. doi: 10.4103/0974-5009.149457 [Crossref] [ Google Scholar]
- Demirkiran F, Yavuz E, Erenel H, Bese T, Arvas M, Sanioglu C. Which is the best technique for endometrial sampling? Aspiration (pipelle) versus dilatation and curettage (D&C). Arch Gynecol Obstet 2012; 286(5):1277-82. doi: 10.1007/s00404-012-2438-8 [Crossref] [ Google Scholar]