Arch Iran Med. 26(1):36-42.
doi: 10.34172/aim.2023.06
Original Article
Effect of Bendopnea on Achievement Medical Treatment Target Doses in Heart Failure
Gülsüm Meral Yılmaz Öztekin Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing, 1, * 
Ahmet Genç Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Resources, Software, Supervision, Validation, Writing – review & editing, 1 
Anıl Şahin Conceptualization, Data curation, Investigation, Methodology, Resources, Supervision, Validation, Writing – review & editing, 2 
Göksel Çağırcı Conceptualization, Supervision, Writing – review & editing, 1 
Şakir Arslan Conceptualization, Supervision, Writing – review & editing, 1 
Author information:
1Department of Cardiology, Antalya Training and Research Hospital, University of Health Sciences, Antalya, Turkey
2Department of Cardiology, Sivas Cumhuriyet University, Sivas, Turkey
Abstract
Background:
The newly described bendopnea in heart failure (HF) is associated with increased cardiac filling pressures. The aim of the study was to show the effect of bendopnea follow-up on reaching optimal medical treatment doses in HF.
Methods:
A total of 413 patients were screened, and we included 203 patients with HF who were previously evaluated for bendopnea. Demographic data, presence or absence of bendopnea, medical history, laboratory findings, and medical treatments were evaluated. Optimal medical therapy target doses at baseline and 3rd month were compared in groups with and without bendopnea.
Results:
On admission, 64 patients (31.5%) had bendopnea. The rate of patients with bendopnea decreased in the 3rd month (n=42, 20.7%). The proportion of patients who used at least 50% of the recommended medical treatment dose on admission and in the 3rd month was compared; angiotensin-converting enzyme inhibitor /angiotensin receptor blockers use increased from 40.6% to 71.9% in those with bendopnea (P=0.013), from 56.1% to 81.3% in those without bendopnea (P<0.001) and beta-blockers use increased from 28.2% to 60.9% in those with bendopnea (P=0.042), from 31.6% to 69.8% in those without bendopnea (P<0.001). However, aldosterone antagonists use decreased from 70.3% to 67.2% in those with bendopnea (P=0.961), from 68.4 % to 64.1% in those without bendopnea (P=0.334). Bendopnea was independently effective in achieving ACE-I/ARB target doses (OR: 0.359, CI 95%: 0.151–0.854, P=0.020).
Conclusion:
Bendopnea follow-up in HF patients can provide a significant improvement in reaching the recommended treatment target doses.
Keywords: Bendopnea, Heart failure, Medical treatment
Copyright and License Information
© 2023 The Author(s).
This is an open-access article distributed under the terms of the Creative Commons Attribution License (
https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article as: Yılmaz Öztekin GM, Genç A, Şahin A, Çağırcı G, Arslan Ş. Effect of bendopnea on achievement medical treatment target doses in heart failure. Arch Iran Med. 2023;26(1):36-42. doi: 10.34172/aim.2023.06
Introduction
Heart failure (HF) affects more than 23 million patients worldwide and causes increased morbidity and mortality.1 Despite significant advances in the treatment of HF, the mortality rate still remains high.2,3
The traditional typical symptoms of HF are shortness of breath, orthopnoea, paroxysmal nocturnal dyspnea, and reduced exercise tolerance. It is recommended that the symptoms and signs of HF should be carefully evaluated at each outpatient visit and treatment changes should be made according to the signs of congestion.4 Bendopnea in HF was first defined in 2014 as shortness of breath on bending forward in less than 30 seconds while wearing or tying shoes.5 Bendopnea is the result of an increase in cardiac filling pressures and is associated with a worse cardiac index and higher right heart pressures.5
The frequency of bendopnea in the general population without HF has been reported as 6.7%.6 While the frequency of bendopnea is 18% in outpatient cases with systolic HF, its frequency increases to 48.8% in decompensated HF.7,8 Bendopnea has been shown to be associated with short-term mortality, especially in advanced New York Heart Association (NYHA) functional class (III and IV).8
HF guidelines recommend the use of angiotensin-converting enzyme inhibitors or angiotensin receptor blockers (ACE-I/ARBs), beta-blockers, aldosterone antagonists, ivabradine, and, more recently, angiotensin receptor–neprilysin inhibitor (ARNI) at maximally tolerated target doses to reduce mortality and/ or rehospitalizations due to HF. These treatment approaches provide better outcomes and survival in HF.4,9 Physicians’ adherence to treatment guidelines was also shown to be a strong predictor of fewer hospitalizations in actual practice.10 However, only 30% of HF patients are treated with the targeted maximum tolerated dose of these drugs.11
As far as we know, there is no article in the literature on the use of bendopnea in the follow-up of HF patients and its relationship with medical treatments. We aimed to show the effect of bendopnea on reaching optimal medical treatment doses at 3 months in HF.
Materials and Methods
Patients aged > 18 years and with a left ventricular ejection fraction (LVEF) ≤ 50% who were followed up regularly were included in the study. Since 2019, bendopnea is routinely evaluated during patient examination in the HF outpatient clinic of our hospital. The presence or absence of bendopnea and onset time are recorded. Bendopnea is evaluated by measuring the time it takes to feel short of breath while sitting in a chair as if tying one’s shoes.5 If there is a symptom before 30 seconds, the presence of bendopnea is considered and the onset time is recorded in the patient’s file. Between February 2019 and March 2020, 413 patients who were evaluated for bendopnea were screened, and 203 patients with at least 3 months of follow-up were included in the study. Patients with severe lung disease were excluded from the study. Sixty-four patients with bendopnea and 139 patients without bendopnea were compared. Demographic data, physical examination, HF symptoms (dyspnea, orthopnea, edema), bendopnea onset time, NYHA functional classification, electrocardiogram, echocardiography, medical history, medical treatments, and laboratory findings were evaluated retrospectively from the clinical database of the HF outpatient clinic. In the 3rd month, the presence of bendopnea, medical treatments, and doses were re-evaluated based on the medical records. All laboratory parameters were measured with standard methods. The SPSS software version 22.0 was used for statistical analysis. Kolmogorov-Smirnov test and Q-Q plot were used for normality. Homogeneity of variance was tested by Levene’s method. Normally distributed results were expressed as means with standard deviations and Student’s t test was used. Non-normally distributed results were expressed as medians and interquartile range (IQR). Number and percentage were used for categorical variables. Continuous variables that were not normally distributed were analyzed by Mann-Whitney U test to compare the clinical features of the groups with and without bendopnea. Chi-square test was used for categorical variables. The chi-square test was used when no more than 20% of the expected numbers were less than 5 and all individual expected counts were 1 or greater. Mean difference and odds ratio estimates with 95% confidence intervals (CIs) were used for the association between bendopnea and medical therapy target doses (with Fisher’s exact test, two-way ANOVA, and Greenhouse–Geisser correction). Multivariate logistic regression analysis was performed to adjust for potential confounders. A P value < 0.05 was considered statistically significant.
Results
The median age of the participants, of whom 69% (n: 140) were male and 31% (n: 63) were female, was 62 years [IQR 55–71]. The median LVEF of patients was 30% [IQR 25–35] and 27% (n: 55) were NYHA functional classes III and IV. Bendopnea was present in 64 of the patients (31.5%) and it was absent in 139 patients (68.5%). The onset time of bendopnea was 18 seconds [IQR 13–25]. Dyspnea was the most common symptom (74.9%, n: 152), followed by orthopnea in 25.1% (n: 51) and edema in 15.8% (n: 32).
The basic characteristics of the patients according to bendopnea status are shown in Table 1. Bendopnea was found more frequently in women than men (P < 0.001). In addition, dyspnea, orthopnea, and edema complaints were observed more frequently in the bendopnea group (P< 0.001). Resting heart rate and atrial fibrillation (AF) rates were slightly higher in those with bendopnea (respectively, P = 0.051, P= 0.057). Most patients with bendopnea were NYHA class III and IV (n:33, 51.6%). When the laboratory findings were compared, albumin and hemoglobin levels were lower in the bendopnea group (respectively, P = 0.003, P < 0.001), while N-terminal pro-brain natriuretic peptide (NT-proBNP) was higher (P = 0.028). C-reactive protein was slightly higher (P= 0.048). Hypertension, diabetes, ischemic etiology and echocardiographic findings were similar between the groups. While the NT-proBNP values of the patients on admission were 1844 [671–3837] ng/L, they decreased to 1200 [453–3097] ng/L in the 3rd month (P = 0.528).
Table 1.
Baseline Characteristics of Heart Failure Patients According to Bendopnea Status
|
Characteristics
|
With Bendopnea (n=64)
|
Without Bendopnea (n=139)
|
P
Value
|
| Age (y) |
65 (58–72) |
62 (54–71) |
0.073 |
| Male, n (%) |
32 (50) |
108 (77.7) |
< 0.001 |
| BMI (kg/m2) |
29 (25–33) |
26 (24–30) |
0.013 |
| HF duration (mon) |
18 (6–84) |
12 (3–42) |
0.093 |
| Dyspnea, n (%) |
62 (96.9) |
90 (64.7) |
< 0.001 |
| Orthopnea, n (%) |
30 (46.9) |
21 (15.1) |
< 0.001 |
| Edema, n (%) |
21 (32.8) |
11 (7.9) |
< 0.001 |
| Ischemic etiology of heart failure, n (%) |
34 (53.1) |
79 (56.8) |
0.621 |
| Medical history |
|
|
|
| Diabetes, n (%) |
26 (40.6) |
51 (36.7) |
0.591 |
| Hypertension, n (%) |
37 (57.8) |
70 (50.4) |
0.323 |
| Atrial fibrillation, n (%) |
17 (26.6) |
19 (13.7) |
0.057 |
| Systolic blood pressure (mm Hg) |
110 (110–120) |
110 (100–130) |
0.684 |
| Diastolic blood pressure (mm Hg) |
60 (60–70) |
60 (60–70) |
0.797 |
| Heart rate (b.p.m) |
82 (68–92) |
74 (65–86) |
0.051 |
| NYHA I, n (%) |
2 (3.1) |
46 (33.1) |
< 0.001 |
| NYHA II, n (%) |
29 (45.3) |
71 (51.1) |
| NYHA III and IV, n (%) |
33 (51.6) |
22 (15.8) |
| Echocardiography |
|
|
|
| LV EDD (mm) |
55 (50–61) |
58 (53–63) |
0.063 |
| LV ESD (mm) |
45 (41–53) |
48 (43–54) |
0.129 |
| PAB (mmHg) |
44 (31–55) |
37 (30–48) |
0.110 |
| LA diameter (mm) |
45 (41–51) |
45 (40–49) |
0.359 |
| LVEF, % |
30 (25–33) |
30 (20–35) |
0.663 |
| Laboratory |
|
|
|
| eGFR (mL/min/1,73 m2) |
66 (48–76) |
69 (53–82) |
0.125 |
| Creatinine (mg/dL) |
1.07 (0.92–1.27) |
1.09 (0.97–1.31) |
0.390 |
| Sodium (mmol/L) |
139 (137–141) |
139 (137–141) |
0.581 |
| Albumin (g/dL) |
4.4 (4–4.6) |
4.6 (4.3–4.8) |
0.003 |
| Haemoglobin (g/dL, mean ± SD) |
12.6 ± 1.69 |
13.6 ± 1.78 |
< 0.001 |
| High sensitive troponin T (ng/L) |
19 (14–34) |
19 (12–32) |
0.568 |
| C-reactive protein (mg/dL) |
5.1 (2.1–12.5) |
3.6 (1.6–8.2) |
0.048 |
| NT-proBNP (ng/L) |
2481 (824–5324) |
1535 (551–3340) |
0.028 |
BMI, body mass index; b.p.m., beats per minute; NYHA, New York Heart Association; LV EDD, left ventricular end-diastolic diameter; LV ESD, left ventricular end-systolic diameter; PAB, pulmonary artery pressure; LA, left atrium; LVEF, left ventricular ejection fraction; eGFR, estimated glomerular filtration rate; NT-proBNP, N-terminal pro-brain natriuretic peptide. Normally distributed data are presented as mean + SD. Non-normally distributed data are presented as median (interquartile range). eGFR was calculated using Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equation.
At the end of the 3rd month, the rate of bendopnea decreased significantly compared to the baseline, and bendopnea was observed in 42 patients (31.5% vs 20.7%, P < 0.001). When the medical treatments recommended by the guidelines were evaluated, 82.3% (n: 167) of all patients were taking ACE-I/ARBs, 90.1% (n: 183) were taking beta-blockers and 74.4% (n: 151) were taking aldosterone antagonists on admission. The rate of medical treatment recommended by the guidelines increased at 3 months compared to baseline. 96.6% (n: 196) of the patients were taking ACE-I/ARBs, 98.5% (n: 200) beta-blockers and 87.2% (n: 177) aldosterone antagonists at the 3rd month (respectively, P < 0.001, P = 0.564, P = 0.002). The proportion of all patients who achieved at least 50% of the target doses in the 3rd month, ACE-I/ARBs (58.4% vs. 78.3%, P< 0.001) and beta-blockers (30.5% vs. 67%, P < 0.001) increased significantly. However, a slight reduction in aldosterone antagonists was also seen (68.9% vs. 65.1%, P = 0.044). The proportion of those receiving less than 50% of the target dose increased from 3.1% to 25% in those with bendopnea and from 5.8% to 20.9% in those without bendopnea compared to baseline (respectively, P= 0.962, P = 0.331). Diuretic use increased from 61.6% to 63.1% (P < 0.001).
The patients who received at least 50% of the treatment target doses recommended by the guidelines followed up with bendopnea were evaluated on admission and 3rd months (Table 2). The proportions of patients receiving at least 50% of the target dose in the bendopnea group increased significantly for ACE-I/ARBs and beta-blockers, but not for aldosterone antagonists (respectively, from 40.6% to 71.9% P = 0.013, from 28.2% to 60.9% P = 0.042, from 70.3% to 67.2%, P = 0.961). ACE-I/ARBs use increased from 56.1% to 81.3% (P< 0.001) and beta-blockers use increased from 31.6% to 69.8% (P< 0.001). However, aldosterone antagonist use decreased from 68.4 % to 64.1% in those without bendopnea (P= 0.334). Loop diuretic use was higher in those with bendopnea at both time points (Table 2). The proportion of patients who received at least 50% of the target dose for ACE-I/ARB increased significantly at 3 months (OR F(1,1):225, 95% CI: 137.9–217.9, P = 0.042) (Table 2). Multivariate logistic regression analysis was performed to adjust for confounders, including bendopnea, age, HF duration, NYHA class, hypertension, education, hospitalization for HF, chronic kidney disease. Bendopnea was independently effective in achieving ACE-I/ARB target doses (OR: 0.359, CI 95%: 0.151–0.854, P = 0.020) (Table 3).
Table 2.
Medical Treatments and NT-proBNP Levels of Heart Failure Patients with and without Bendopnea on Admission and at 3rd Month
|
Medications
|
On Admission
|
P
Value
|
At 3rd Month
|
P
Value
|
OR (95% CI)
|
P
Value
|
|
With Bendopnea
|
Without Bendopnea
|
With Bendopnea
|
Without Bendopnea
|
| ACE-I/ARB, n (%) |
46 (71.9) |
121 (87.1) |
0.009 |
60 (93.8) |
136(97.8) |
0.138 |
0.861 (0.549–1.358) |
0.563 |
| < 50% target doses |
20 (31.3) |
42 (30.2) |
0.041 |
14 (21.9) |
23 (16.5) |
0.287 |
F(1,1):225 (137.9–217.9) |
0.042 |
| ≥ %50 target doses |
26 (40.6) |
78 (56,1) |
46 (71.9) |
113 (81.3) |
| Beta-blockers, n (%) |
56 (87.5) |
127 (91.4) |
0.390 |
62 (96.8) |
138 (99.3) |
0.187 |
1.449 (0.899–2.308) |
0.125 |
| < 50% target doses |
37 (57.8) |
82 (59) |
0.626 |
23 (35.9) |
41 (29.5) |
0.420 |
F(1,1):0.526 (17.44–55.56) |
0.600 |
| ≥ %50 target doses |
18 (28.2) |
44 (31.6) |
39 (60.9) |
97 (69.8) |
| Loop diuretics, n (%) |
48 (75) |
77 (55.4) |
0.008 |
49 (76.6) |
79 (56.8) |
0.007 |
1.263 (0.737-2.107) |
0.423 |
| Aldosterone antagonist, n (%) |
47 (73.4) |
104 (74.8) |
0.834 |
59 (92.2) |
118 (84.9) |
0.148 |
0.903(0.572–1.455) |
0.722 |
| < 50% target doses |
2 (3.1) |
8 (5.8) |
0.423 |
16 (25) |
29 (20.9) |
0.424 |
F(1,1):25 (111.9–65.94) |
0.125 |
| ≥ %50 target doses |
45 (70.3) |
95 (68.4) |
43 (67.2) |
89 (64.1) |
| ARNI, n (%) |
4 (6,3) |
2 (1.4) |
0.060 |
4 (6,3) |
2 (1.4) |
0.060 |
|
|
| NT-proBNP (ng/L) |
2481
(823–5324) |
1535
(550–3340) |
0.028 |
1632
(504–3555) |
1165
(420–2909) |
0.117 |
|
|
ACE-I, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; ARNI, angiotensin receptor/neprilysin inhibitor; NT-proBNP, N-terminal pro-brain natriuretic peptide; OR, odds ratio; CI, confidence interval.
Table 3.
Multivariable Logistic Regression for Potential Confounders Related to Reaching the Medical Therapy Target Doses
|
Variables
|
ACE-I/ARB
|
Beta-Blocker
|
Aldosterone Antagonist
|
|
β
|
OR (95% CI)
|
P
Value
|
β
|
OR (95% CI)
|
P
Value
|
β
|
OR (95% CI)
|
P
Value
|
| Bendopnea |
-1.025 |
0.359 (0.151–0.854) |
0.020 |
0.077 |
1.080 (0.450–2.590) |
0.863 |
-0.176 |
0.839 (0.330–2.132) |
0.712 |
| Age |
-0.003 |
0.997 (0.967–1.028) |
0.850 |
-0.009 |
0.991 (0.960–1.023) |
0.575 |
-0.025 |
0.975(0.941–1.011) |
0.169 |
| HF duration |
-0.004 |
0.996 (0.988–1.003) |
0.263 |
0.002 |
1.002 (0.995–1.010) |
0.513 |
0.000 |
1.000(0.992–1.011) |
0.943 |
| NYHA class |
0.496 |
1.642 (0.654–4.124) |
0291 |
-0.266 |
0.766 (0.293–2.007) |
0.588 |
-0.381 |
0.683 (0.253–1.848) |
0.453 |
| Hypertension |
0.581 |
1.788 (0.839–3.811) |
0.132 |
0.728 |
2.071 (0.932–4.603) |
0.074 |
-0.778 |
0.459 (0.201–1.050) |
0.065 |
| Education |
1.261 |
3.528(0.471–26.427) |
0.220 |
1.485 |
4.416 (0.574–33.977) |
0.552 |
0.210 |
1.234 (0.142–10.752) |
0.849 |
| Hospitalization for HF |
0.364 |
1.439 (0.864–2.397) |
0.162 |
0.027 |
1.028 (0.608–1.738) |
0.919 |
0.142 |
1.152 (0.676–1.964) |
0.602 |
| Chronic kidney disease |
-0.645 |
0.525 (0.145–1.902) |
0.326 |
-0.658 |
0.518 (0.131–2.044) |
0.347 |
-1.351 |
0.259 (0.072–0.929) |
0.038 |
ACE-I, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; OR, odds ratio; CI, confidence interval; HF, heart failure; NYHA, New York Heart Association.
The medical treatments and NT-proBNP levels of the patients on admission and the 3rd month according to bendopnea status are shown in Figure 1. The use of ACE-I/ARBs was significantly lower in those with bendopnea on admission in both groups. However, the rate of using beta blockers and aldosterone antagonists was similar. In the 3rd month, the rate of ACE-I/ARBs, beta-blockers, and aldosterone antagonists increased similarly in both the bendopnea and non-bendopnea groups (Figure 1). NT-proBNP levels were higher in the bendopnea group on admission (P= 0.028); and decreased in both groups in the 3rd month. However, it was similar in the two groups (P = 0.117) (Table 2 and Figure 2).
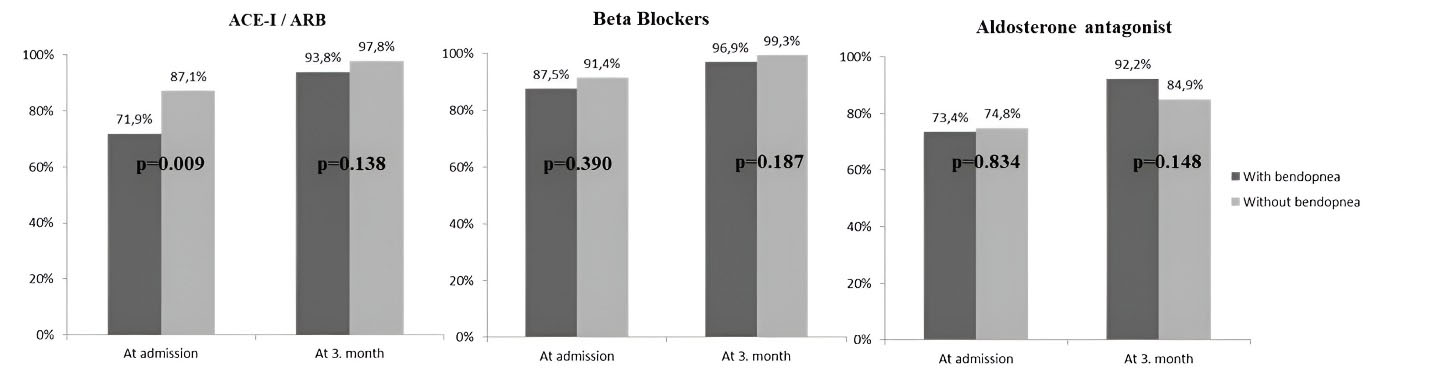
Figure 1.
Medical Treatments of Heart Failure Patients with and without Bendopnea on Admission and at 3rd Month. (ACE-I/ARB, angiotensin-converting enzyme inhibitor/angiotensin receptor blocker)
.
Medical Treatments of Heart Failure Patients with and without Bendopnea on Admission and at 3rd Month. (ACE-I/ARB, angiotensin-converting enzyme inhibitor/angiotensin receptor blocker)
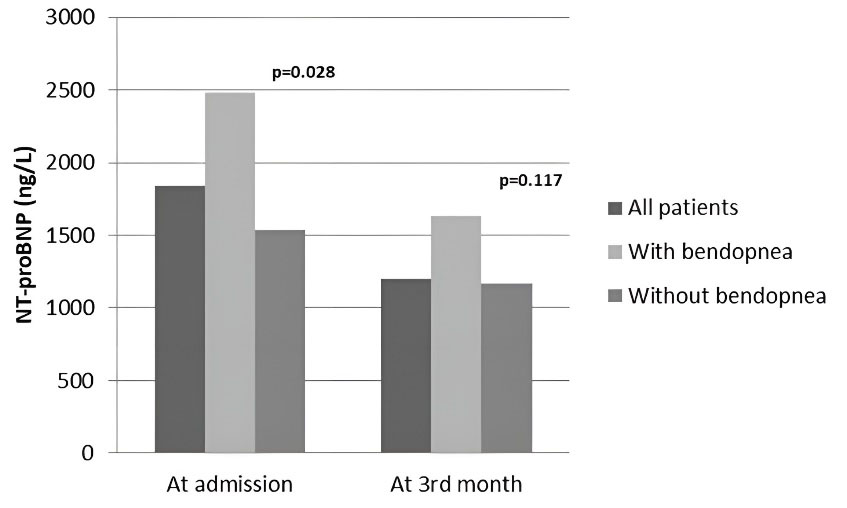
Figure 2.
NT-proBNP levels of Patients with and without Bendopnea at Admission and 3rd Month. (NT-proBNP, N-terminal pro-brain natriuretic peptide)
.
NT-proBNP levels of Patients with and without Bendopnea at Admission and 3rd Month. (NT-proBNP, N-terminal pro-brain natriuretic peptide)
Discussion
In this study, we reported that the evaluation of bendopnea in the follow-up of HF can provide a significant improvement in reaching the recommended medical treatment doses. The bendopnea rate decreased from 31.5% to 20.7% at the end of 3 months of follow-up. At 3 months, the rate of reaching at least 50% of the target doses of ACE-I/ARBs and beta-blockers, which are known to reduce mortality, increased significantly. The proportion of patients who received at least 50% of the target dose for ACE-I/ARB increased significantly at 3 months. Bendopnea was independently effective in achieving ACE-I/ARB target doses in multivariate analyses. Evaluation of bendopnea in the follow-up of HF patients can provide a stronger idea about the congestion status and filling pressures. Therefore, assessment of bendopnea may compel clinicians to achieve optimal medical therapy doses of HF treatments.
Dyspnea that occurs within 30 seconds of bending forward while putting on or tying shoes has been recently reported in 2014 as a new symptom called bendopnea in HF. The already high ventricular filling pressure in HF patients is further increased by this maneuver.5 The study by Thibodeau et al included mostly elderly patients (mean age 81.8 years), with a frequency of approximately 48.8% and a mean time of onset of bendopnea of 13.4 seconds ( ± 6.9).5 In our study, the median age was 62 years, the frequency of bendopnea was 31.5%, and the onset time of bendopnea was 18 seconds [IQR 13-25]. With age, the frequency of bendopnea may increase and the onset of shortness of breath may be earlier. However, it is necessary to carry out studies specific to age ranges to support this notion. Because that study included patients presenting with decompensated HF, the frequency was higher compared to our study, which included more stable outpatients. In another study with stable ambulatory HF, bendopnea was reported with a lower frequency (18%).7
Dyspnea was the most common symptom in our study population (74.9%), and this rate was higher in those with bendopnea (96.9%). Orthopnea was present in 46.9% and edema in 32.8% of patients with bendopnea. Although this rate was lower than the study on patients with decompensated HF (59% and 70.5%, respectively), it was significantly higher than patients without bendopnea. The patients with bendopnea described dyspnea as the most frequent symptom, at 99.2%.8 While dyspnea is reported as the most common symptom of hospitalization, paroxysmal nocturnal dyspnea is associated with increased left ventricle filling pressures.12,13 Edema is one of the most common symptoms of decompensated HF, but several noncardiac causes can produce it.12 In a meta-analysis, there was an association between bendopnea, dyspnea, orthopnea, and paroxysmal nocturnal dyspnea.14 Dyspnea, orthopnea and edema complaints were more common in patients with bendopnea in our study, too. Therefore, we believe that the evaluation of the presence of bendopnea can provide more objective data about the increase in filling pressures.
Similarly, in previous studies, hypertension and diabetes were not associated with bendopnea.5 The presence of AF and heart rate was slightly higher in patients with bendopnea in our study. Confirming this, bendopnea shows more symptomatic patients. The interaction between body mass index (BMI) and bendopnea is not clear. In our study and the first bendopnea study with higher BMI values, BMI and bendopnea were found to be associated.5 However, in another study with similar BMI values to our study, no relationship was found with bendopnea.9
More than half of HF patients with bendopnea were in NYHA class III and IV in our study. Similarly, bendopnea has been previously associated with functional class NYHA III and IV, indicating it is a symptom of advanced HF.5,7 However, physical examination is essential in the diagnosis and treatment of HF and can provide as much insight into cardiac filling pressures as brain natriuretic peptides.4 NT-proBNP levels were higher in the bendopnea group on admission. At 3 months, this difference disappeared and there was a similar decrease in NT-proBNP values in both groups. Therefore, we believe that bendopnea evaluated together with NYHA classes and NT-proBNP can yield a better idea about filling pressures.
In a previous study, the rates of ACE-I/ARBs, beta-blockers, and mineralocorticoid receptor antagonists used in the outpatient population with HF with reduced LVEF were 90.5%, 87.8%, and 42.7%, respectively, but the number of patients using drugs at the target dose was below 50%,15 whereas the same rates were 82.3%, 90.1%, and 74.4%, respectively, in our study. However, in our follow-up, the rate of patients who received 50% of the target dose increased significantly in ACE-I/ARBs and beta-blockers compared to admission (respectively, 58.4% vs. 78.3%, P < 0.001, 30.5% vs. 67%, P < 0.001). There was a significant reduction for the aldosterone antagonists (68.9% vs. 65.1%, P = 0.044). The proportion of those who received less than 50% of the target dose of aldosterone antagonists increased from baseline in both those with and without bendopnea. This may be due to higher doses of ACE-I/ARB in follow-up and the reduction or discontinuation of aldosterone antagonists due to the resulting hyperkalemia.
As far as we know, the doses of HF treatments and the proportion of patients reaching the target dose in patient groups with and without bendopnea have not been reported before. In the 3rd month, the rate of use of ACE-I/ARBs, beta-blockers, and aldosterone antagonists increased in all patients with and without bendopnea. The proportion of those who received ACE-I/ARBs and at least 50% of the target dose was significantly lower in the bendopnea group both on admission and in the 3rd month. More loop diuretics were used in patients with bendopnea at both time points, as it was associated with higher filling pressures. However, in the first study on bendopnea, medical treatment rates were similar between the groups with and without bendopnea, including diuretics.5 In a study on outpatient cases with systolic HF, the rates of non-diuretic treatments were found to be similar between the groups with and without bendopnea.7 Also, the rate of aldosterone antagonist use in our study was 93.3%, while it was approximately 50% in the other two studies.5,7 In our study, the rate of those who received at least 50% of the target dose of ACE-I/ARBs and beta-blockers at 3 months increased in HF patients with and without bendopnea.
Our study had several limitations. The number of patients was limited since the study was retrospectively planned in a single center and patients previously evaluated for bendopnea were included. A prospective study with a longer follow-up period can be performed with a larger number of patients. In our study, treatments were directed based on NYHA classes or NT-proBNP levels or bendopnea status during follow-up and the rates of reaching the target dose were not compared. Since our study was a retrospective observational study, we could not provide these data. Prospective studies can be planned to compare HF follow-up methods and determine which one is more applicable. Since the LVEF of the patients in our study was ≤ 40%, there is insufficient data for HF with mid-range and preserved LVEF. It is difficult to determine which drug has a greater bendopnea-reducing effect, as it is recommended to start with these drugs that reduce mortality in HF treatment guidelines. Such an evaluation could not be made because the drugs were not started separately.
In conclusion,the use of bendopnea in the follow-up of HF patients can provide an objective understanding of the severity of symptoms. We also believe that it may be challenging for us to reach optimal medical treatment doses. Evaluation of bendopnea in addition to symptoms, NYHA classes, and NT-proBNP levels during follow-up can provide objective data in patient follow-up and accelerate the achievement of treatment goals.
Competing Interests
All authors declare that they have no conflicts of interest.
Ethical Approval
Approval was obtained from Antalya Training and Research Hospital Ethical Committee (Date: 08/07/2021, Decision No. 10/7).
Funding
All authors declare that they have no financial disclosure.
References
- Dunlay SM, Roger VL. Understanding the epidemic of heart failure: past, present, and future. Curr Heart Fail Rep 2014; 11(4):404-15. doi: 10.1007/s11897-014-0220-x [Crossref] [ Google Scholar]
- Shahar E, Lee S, Kim J, Duval S, Barber C, Luepker RV. Hospitalized heart failure: rates and long-term mortality. J Card Fail 2004; 10(5):374-9. doi: 10.1016/j.cardfail.2004.02.003 [Crossref] [ Google Scholar]
- Spencer FA, Meyer TE, Goldberg RJ, Yarzebski J, Hatton M, Lessard D. Twenty year trends (1975-1995) in the incidence, in-hospital and long-term death rates associated with heart failure complicating acute myocardial infarction: a community-wide perspective. J Am Coll Cardiol 1999; 34(5):1378-87. doi: 10.1016/s0735-1097(99)00390-3 [Crossref] [ Google Scholar]
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J 2016; 37(27):2129-200. doi: 10.1093/eurheartj/ehw128 [Crossref] [ Google Scholar]
- Thibodeau JT, Turer AT, Gualano SK, Ayers CR, Velez-Martinez M, Mishkin JD. Characterization of a novel symptom of advanced heart failure: bendopnea. JACC Heart Fail 2014; 2(1):24-31. doi: 10.1016/j.jchf.2013.07.009 [Crossref] [ Google Scholar]
- Baeza-Trinidad R, Isaula-Jimenez O, Peinado-Adiego C, Mosquera-Lozano JD. Prevalence of bendopnea in general population without heart failure. Eur J Intern Med 2018; 50:e21-e2. doi: 10.1016/j.ejim.2017.11.007 [Crossref] [ Google Scholar]
- Thibodeau JT, Jenny BE, Maduka JO, Divanji PH, Ayers CR, Araj F. Bendopnea and risk of adverse clinical outcomes in ambulatory patients with systolic heart failure. Am Heart J 2017; 183:102-7. doi: 10.1016/j.ahj.2016.09.011 [Crossref] [ Google Scholar]
- Baeza-Trinidad R, Mosquera-Lozano JD, El Bikri L. Assessment of bendopnea impact on decompensated heart failure. Eur J Heart Fail 2017; 19(1):111-5. doi: 10.1002/ejhf.610 [Crossref] [ Google Scholar]
- Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Drazner MH. 2013 ACCF/AHA guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation 2013; 128(16):1810-52. doi: 10.1161/CIR.0b013e31829e8807 [Crossref] [ Google Scholar]
- Komajda M, Lapuerta P, Hermans N, Gonzalez-Juanatey JR, van Veldhuisen DJ, Erdmann E. Adherence to guidelines is a predictor of outcome in chronic heart failure: the MAHLER survey. Eur Heart J 2005; 26(16):1653-9. doi: 10.1093/eurheartj/ehi251 [Crossref] [ Google Scholar]
- Maggioni AP, Anker SD, Dahlström U, Filippatos G, Ponikowski P, Zannad F. Are hospitalized or ambulatory patients with heart failure treated in accordance with European Society of Cardiology guidelines? Evidence from 12,440 patients of the ESC Heart Failure Long-Term Registry. Eur J Heart Fail 2013; 15(10):1173-84. doi: 10.1093/eurjhf/hft134 [Crossref] [ Google Scholar]
- Kato M, Stevenson LW, Palardy M, Campbell PM, May CW, Lakdawala NK. The worst symptom as defined by patients during heart failure hospitalization: implications for response to therapy. J Card Fail 2012; 18(7):524-33. doi: 10.1016/j.cardfail.2012.04.012 [Crossref] [ Google Scholar]
- Watson RD, Gibbs CR, Lip GY. ABC of heart failure Clinical features and complications. BMJ 2000; 320(7229):236-9. doi: 10.1136/bmj.320.7229.236 [Crossref] [ Google Scholar]
- Pranata R, Yonas E, Chintya V, Alkatiri AA, Budi Siswanto B. Clinical significance of bendopnea in heart failure-Systematic review and meta-analysis. Indian Heart J 2019; 71(3):277-83. doi: 10.1016/j.ihj.2019.05.001 [Crossref] [ Google Scholar]
- Poelzl G, Altenberger J, Pacher R, Ebner CH, Wieser M, Winter A. Dose matters! Optimisation of guideline adherence is associated with lower mortality in stable patients with chronic heart failure. Int J Cardiol 2014; 175(1):83-9. doi: 10.1016/j.ijcard.2014.04.255 [Crossref] [ Google Scholar]